Disaster Preparedness
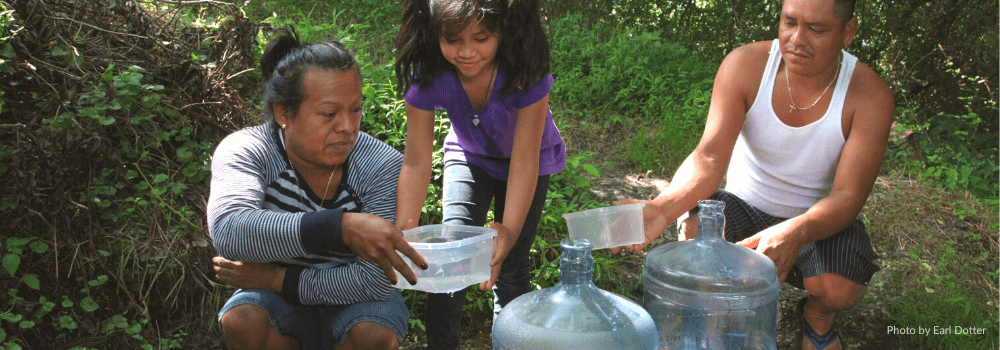
The impact of disasters and other major weather events can vary greatly.
These events amplify preexisting struggles that many in our community have. This is particularly evident during major disasters. Some members of our communities – due to individual characteristics including geographic remoteness, language, heritage, poverty, medical issues, among others – are frequently unaccounted for when a disaster strikes. Communities need to prepare for disasters, and build plans for response and recovery, with all members of the community brought to the table. MCN’s disaster preparedness initiative seeks to provide training, technical assistance, resources, and strategies to communities and community health centers (CHCs) for hyperlocal, hyper-inclusive responses to major natural events.
Our History Working with Communities Affected by Disasters
MCN facilitates robust CHC emergency management planning; builds community engagement by bringing in community leaders to develop, review, and strengthen emergency action plans; and identifies and engages vulnerable populations like farmworkers, children, and isolated rural residents. But we aren’t just bringing partners together; we’re enabling stronger, healthier communities. For example, we’ve learned plans must address the mental health and psychosocial needs of both community members and CHC staff impacted by disasters. One tactic we offer is a natural hazards intervention to build tools and resources for educating CHCs on the screening, monitoring, and evaluation of the different aspects that need to be assessed when it comes to major disasters including mental health and the ability to recover and prepare for new events.
Community Health Centers Lead Emergency Response
We activate our 40 years of providing training and technical assistance to CHCs to guide them in expanding their reach to the most vulnerable. CHCs, with emergency infrastructure including generators and with mandated emergency plans already in place, can be key anchors to steady the community as the focal point for community mobilization during and after a major event. While CHCs are tasked to prepare for typical emergencies within their walls, our new efforts: 1) pull clinicians out into the community and prioritize recognition of and care for those who are often overlooked or have limited care access; and 2) acknowledge natural hazards and expand emergency preparedness to adapt to changes in the environment or the population.
Best Practices: How we support communities and health centers in addressing disasters and major events.
|
|
|
Our Research: Increasing Resilience
MCN is exploring the impact of major events and public health emergencies on agricultural workers and their families in central Puerto Rico. Understanding the impact and the social factors influencing them is essential for policymakers, clinicians, worker groups, and other stakeholders. Through these projects, we are working with CHCs, schools, and community leaders in the region to address the gaps, needs, and challenges when implementing emergency resiliency initiatives. In addition, knowing the effect of recent emergencies and disasters on agricultural workers’ children can help them design evidence-based intervention strategies, and prevention programs.
|
|
Learn More About Our Efforts
Peer-Reviewed Publications 2022
- Pagán-Santana M, Liebman AK, López-Correa AY. Looking at the gaps and program needs to address the impact on children of agricultural workers in Puerto Rico during and after public health emergencies. Front Public Health. 2022 Nov 7;10:1046701. doi: 10.3389/fpubh.2022.1046701. PMID: 36419994; PMCID: PMC9677091.
- Grzywacz JG, Gonzales-Backen M, Liebman A, Marín AJ, Trejo M, Gudino CO, Economos J, Tovar-Aguilar JA. Attending to Pesticide Exposure and Heat Illness Among Farmworkers: Results From an Attention Placebo-Controlled Evaluation Design. J Occup Environ Med. September 2019. doi: 10.1097/JOM.0000000000001650.
Other Resources
- Heat-Related Illness Clinician’s Guide (Available in English and Spanish)
- Environmental Education [Videos, Resources and Curriculum] (Available in English and Spanish)
- Heat-related Illness and Farmworkers - Training Curriculum and Facilitator Guide (Available in English and Spanish)
- Heat-related Illness Webpage (View MCN's heat-related illness webpage for more resources)
Advocacy and Media
- Regional Heat Stress Standard to Protect Workers
- Calling for Federal Heat Standard for Workers
- Protecting Farmworkers from Heat
Learning Opportunities
- It’s Hot and It’s Dangerous! A Webinar for Community Health Workers to Learn about Heat Related-Illness and How to Help Prevent It. [Recorded Webinar ENG]
- Antes de los días de verano, aprenda cómo los Promotores de Salud pueden ayudar en prevenir enfermedades a causa del calor

