COVID-19 Vaccine for Refugees, Immigrants, and Migrants: Building Trust on the Frontlines
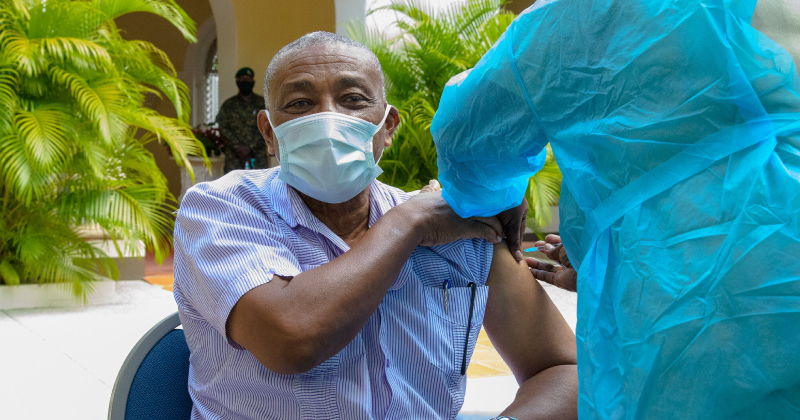
Last month, experts in migrant health gathered as panelists on MCN’s webinar, COVID-19 Vaccines: A National Learning Session from the Frontlines of Refugee, Migrant, and Immigrant Health. Sharing challenges and best practices from their frontline experiences, the panelists discussed how to improve refugee, immigrant, and migrant (RIM) communities’ access to COVID-19 vaccines through building trust and being in touch with the needs of unique vulnerable communities. Special focus was given to essential worker patients who are included in many states’ early phases of vaccine rollout.
Vaccine Hesitancy: The Fight Against Misinformation
Before COVID-19 vaccines became available, health care organizations had been concerned about the influence of vaccine hesitancy on the public’s acceptance of the COVID-19 vaccine. While there has been dialogue about the influence of misinformation and conspiracy theories on perceptions of the COVID-19 vaccines, there are also justifiable public concerns about the vaccines, especially for vulnerable populations. Andrea Caracostis, MD, MPH, Executive Director of the HOPE Clinic, a federally qualified health center providing care to the large multicultural community in Southwest Houston, Texas explained that the US population needs to be given the “benefit of a doubt” that some of their hesitancy is due to the vaccines’ newness. Lynn Bahta, RN, MPH, CPH, a public health nurse at the Minnesota Department of Health, also noted that she has learned through her work as a subject matter expert on vaccine hesitancy, that one of the most common concerns about the COVID-19 vaccine across various populations spurs from the fact that the vaccine was created very quickly. Yet, still, vulnerable immigrant populations and populations of color have other justifiable concerns that are unique from the general US population. Panelist Eva Gálvez, MD, family physician at Virginia Garcia Memorial Health Center and Board Chair for Migrant Clinicians Network explained that some of the hesitancy for immigrants and migrants to the US comes from the US’s negative history with unethical uses of vaccines on populations of color.
Beyond these reasonable concerns, misinformation is the cause of much hesitancy as well, and comes in a variety of forms. Bahta explained that over the years she has seen misinformation about various vaccines disseminated through campaigns, including those using pamphlets, the internet, and social media. However, the most common, and perhaps the most dangerous, kind of misinformation, is the kind that is communicated from word of mouth. Dr. Gálvez shared that she has heard many kinds of hesitancies amongst her patients. Some patients are worried about dangerous side effects, or whether the vaccines will have long-term risks. Dr. Gálvez explained that these concerns are coming from social media as well as from word-of-mouth communication with family and friends in other countries. “Many of our patients are really connected to their families back home through social media and video chat. It is definitely influencing them,” she argues. Conspiracy theories such as fears about the vaccine being a method for the government to control the population or alter the DNA of communities of color has been communicated to her as well. Some of her patients express fear of the hospital system as a result of the negative experiences of their families in Mexico, who have heard of stories of people they know having gone into hospitals and not come out, causing hospitals to be alternatively called “death camps”. This general feeling that hospitals may be killing patients, intentionally or unintentionally, alters her patients’ trust in health care. She presses that these fears are amplified by the US health care system and government systems’ anti-immigrant policies and rhetoric that is “raising peoples’ fear and suspicion.”
Dr. Caracostis explained that communicating through the channels patients use, such as social media, is important. “That is how they relate to other countries…. They want to keep connected to their cultures and information gets transmitted that way,” she said. While it may be easy for most doctors to direct their patients to find reputable sources of information rather than turning to friends and family, Dr. Gálvez explained that many immigrants do not have access to information in their language and in a format they can understand.
Barriers to Vaccine Access
From a place of vaccine hesitancy, vulnerable populations need easy access to information and COVID-19 vaccines, both of which, as the panelists explained, are difficult to come by. Immigrants often face challenging disproportionate barriers to access the vaccine, as well as disproportionate risks to being infected with COVID-19.
Information Barriers
Bahta, drawing from her 20 years of experience with immunizations and vaccine hesitancy, stressed that fighting against misinformation requires creating good information, and getting people access to that information, just as quickly as the misinformation is disseminated. However, Dr. Caracostis points out that one failure of health centers is the habit of simply translating informational documents that often miss addressing the unique questions and concerns of their community members.
Lourdes Villanueva, Director of Farmworker Advocacy at Florida’s Redlands Christian Migrant Association (RCMA), shared the perilous struggles of the farmworker families her community organization serves during COVID-19. These struggles included RCMA families not having access to sick pay, having to continue driving to work as early as 5am without adequate documentation, against COVID-19 curfew, and not having access to COVID-19 testing. Villanueva recollects one rural area which did not receive any testing until June 15 – months into the pandemic. While vaccines are not yet available in her community, Villanueva hopes that the farmworker families will not have to suffer limited access to COVID-19 vaccines as time goes on. Because RCMA has not received commitments from Florida that vulnerable essential workers will be prioritized for COVID-19 vaccine distribution, she fears that once the harvesting season in Florida ends, workers will bring COVID-19 to other areas of the US. When vaccines do reach RCMA’s communities they will face a challenge that is surfacing across the US: the request for identification. Villanueva explained that often, COVID-19 testing sites asked her families for proof of residency, like identification cards. Many RCMA families do not have documentation and may not understand that proof of residency did not mean they needed to provide their immigration status. To attempt to fix this issue, Villanueva worked with a lawyer to help get workers in RCMA families identification cards for residency. However, this issue must be fixed at a mass level. RCMA is currently working with the state to address this issue as well as clarification issues with other policies surrounding the COVID-19 vaccines to increase vaccine access. Villanueva is also working with farm owners to provide temporary residency documentation to their workers.
Barriers to Receiving COVID-19 Vaccines
As Villanueva highlighted, the need for clear information is high. Dr. Gálvez shared additional barriers she has encountered that have made inclusive rollout strategies a challenge to achieve on the frontlines. Dr. Gálvez noted that individual state regulations for rollout population order was one barrier to COVID-19 vaccine access. While essential workers are prioritized in some states, in Oregon, where she practices, other population groups are prioritized, bumping down essential workers and even the elderly. Other barriers include having to sign up for vaccines online, requiring access to a computer, internet, and a level of technological literacy. Another access barrier Dr. Gálvez has encountered is extended distances to vaccine dissemination sites, which cause increased disadvantages for those with limited transportation.
Best Practices for Equitable COVID-19 Vaccine Rollout
As panelists shared the best practices of their frontline health centers and community groups, a common theme emerged: the need for advocacy and community engagement at each step in the process of successful vaccine access for vulnerable refugee, migrant, and immigrant populations.
Reducing Vaccine Hesitancy
While the COVID-19 vaccines are still fairly new, community-focused steps can be taken to decrease hesitancy and other challenging barriers to the vaccine. For example, Dr. Caracostis encourages clinicians to lead by example to inspire community leaders to get vaccinated. Community leaders can help decrease vaccine hesitancy by talking favorably about the vaccine. Dr. Caracostis feels this kind of method has helped the HOPE clinic vaccinate about 70 percent of their staff. While a staff survey had shown only 50 percent of staff had originally wanted to be vaccinated, after the first wave of vaccinations, and after staff members who were vaccinated proudly showed off the bandage on their arm where they received the shot, many more staff members wanted to be vaccinated for the offices’ second round. Dr. Caracostis is confident many more staff will get the vaccine by their third.
To combat specific vaccine hesitancies, such as those related to the speed of COVID-19 vaccine creation, Bahta recommends having talking points when talking to community members which explain reasons why vaccines were able to be created quickly (such as the immense funds put towards the creation of vaccines, and the 20 years of pre-clinical vaccine research that had already been conducted). Bahta noted that hesitancy related to “historical and current racial injustices” within one’s community may be overcome through the acknowledgement of fears and open conversations with community members, “so they have a chance to express their concerns and frustrations with the system,” she explained. She said that conversations like these may lead to discussions and willing ears to hear information the health center has to offer.
On-Target Messaging
Bahta explained she has learned through frontline experience that some vulnerable populations have limited access to both reliable information and dialogue. She noted that it is easy for health centers to simply create messaging in the language of the vulnerable population they are trying to reach, like her health department did in 2009 when they were trying to reach Minnesota Somali populations. “It was great information, but it did not resonate in the community,” she noted. Yet after advocating for local Somali populations to her managers, requesting that a Somali community member be hired to help, hesitancy within the community began to disappear. Through their community engagement, they found differing opinions within the local Somali community. Interviews with community members in Somali allowed “cultural innuendos” to be used and understood. When a measles outbreak occurred in 2017, which included a disproportionate percentage of the local Somali population, Somali community members on staff and a pre-existing advocacy group for public health helped create on-target messaging to relatively quickly resolve the measles outbreak.
Bahta emphasized that those who were most familiar with the community should create messaging, and those who may find themselves in positions of power, as a public health authority, due to white privilege, or from both, have a duty to elevate the voices of those who are actively engaged in and part of the community. Another important lesson she learned was to “be nimble in expectations” while allowing others to take control. She warned that expectations in public health are often “driven by the system and not driven by what is actually effective in a community of people.”
Equitable Access to COVID-19 Vaccines
Once hesitancy is diminished, it is important to ensure equitable access to vaccines. Dr. Caracostis shared how HOPE Clinic conducted a special event for 500 Vietnamese seniors as efficiently and equitably as possible. All patients were signed up ahead of time, forms were translated, and interpreters were provided throughout the event. Providers also ‘championed’ the idea of getting vaccinated to their patient community, who trusted them. While Dr. Caracostis was happy about the success of their events, she shared her concern about getting people excited about the vaccine when they have such a limited supply. “Sometimes if people can’t get the vaccine when they want it, they may give up on getting it all together” she said. When asked whether she would be concerned if someone outside of her service populations wanted to get a vaccine from their clinic, she said, “No, never. I think we have to vaccinate everybody that wants a vaccine, as soon as possible.” Partnering with other organizations, including the coordination of transfer of unused vaccine to another clinic’s patient community, is another important consideration she shared.
CDC’s COVID-19 Vaccine Rollout Recommendations in English and Spanish
Q&A: What PCPs need to know about COVID-19 vaccines in English
A Checklist for COVID-19 Vaccine Roll-out among Refugees, Immigrants, and Migrants in English
COVID-19 Vaccines: Health Department and Vaccine Clinic Considerations to Reach Migrant and Immigrant Workers in English and Spanish
PSA COVID-19 Vaccine: Dr. Eva Galvez, a physician serving migrant and immigrant communities in English and Spanish
Interview on COVID-19 Vaccine: Dr. Eva Galvez, a physician serving migrant and immigrant communities in English and Spanish
Like what you see? Amplify our collective voice with a contribution.
Got some good news to share? Contact us on our social media pages above.
Return to the main blog page or sign up for blog updates here.
- Log in to post comments