Anna and Annie, the Nurse Midwives, Greet Pregnant Asylum Seekers with Empathy and Care

Annie Leone, CNM, welcomes new arrivals at the center.
“Midwives have always been on the forefront of justice for women and reproductive justice. Our profession is at the forefront of this. This community of migrants, there’s a lot that they are facing. It makes sense for midwives to take care of this community.” – Annie Leone, CNM
[Editor’s Note: Tomorrow is International Day of the Midwife! This special day has been observed for over 30 years on May 5th, just a few days before Mother’s Day. Migrant Clinicians Network works with midwives Anna Haas, CNM and Annie Leone, CNM at the US-Mexico border to triage pregnant people after they have been released from detention and sign them up with Health Network to connect them with prenatal care in their receiving community, through the Healthy Babies, Children, and Mothers project.]
When expecting parents cross the border and are released from detention to an immigration shelter, immediate care is vital to guarantee a quick response to any pregnancy complications and to help these pregnant asylum seekers prepare for their upcoming deliveries. Many of these asylum seekers have experienced a long hard trek and difficulties in crossing the border. Most have had little to no prenatal care. Yet, few receive any medical attention at the border; many immigration shelters do not have the funding to provide it. Additionally, it is important to greet them in a language they know and to welcome them with empathy and care and help them get linked into a system of care at their next destination so that their pregnancies can be healthy. This is where Anna Haas, CNM, and Annie Leone, CNM, come in.
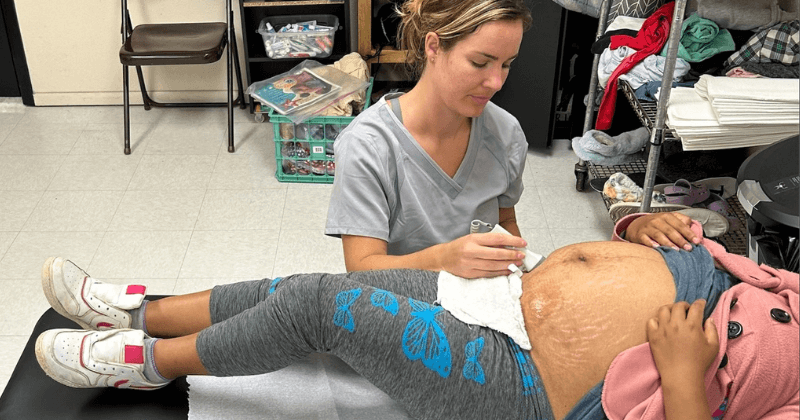
Anna Haas, CNM, provides a check-up to a new arrival.
As bilingual certified nurse midwives, Haas and Leone are prepared not just to help with medical needs, but to welcome people into this country. Their efforts are supported by a partnership between Holy Family Birth Center, Migrant Clinicians Network, Catholic Charities Respite Center, Community for Children, and Every Mother Counts. Haas and Leone care for hundreds of pregnant people each year and enroll many into MCN’s Health Network program to help connect them with needed prenatal and perinatal care. The two midwives work closely with Health Network Associates Brenda Ramirez and Enedelia “Ene” Basurto at the shelter.
“Every day there are new stories. We provide them an opportunity to talk about their stories,” said Leone. Midwives can listen to pregnant asylum seekers and provide support that is essential for their overall well-being, she noted. “I ask them why they leave their countries, and it seems clear to me that no one has asked them this at this point. No one who is there to process them, receive them, has asked them this. People want to share their stories. They are happily surprised to see someone ask them. This allows us to make a deeper connection and we can better understand their needs. There is a lot of trauma and fear in this community. Midwives’ philosophy of caring for the whole person is unique.”

MCN provides resources and information to those arriving at the center.
“Every day is a little different with how many patients we see,” said Haas. “We’re usually there morning to evening and there are always people coming in. We see pregnant and postpartum patients, [in addition to providing] some primary care. When we go there, we announce to the people that if they are pregnant or recently had a kid they can come and be seen. At the clinic we do a quick visit; it can be longer depending on what’s going on with the patient. We do a quick exam on the mom, check the vitals of the mom and the baby. If there’s something going on with the mom, we organize transport to take her over to a hospital if she needs to go.” Mothers and babies are also given clean clothes and an opportunity to rest and recover at this time.
In one day at the shelter, the two midwives may see anywhere between ten to 25 patients. After their exams, the midwives provide needed medication or vitamins at no cost to the patient. They write prescriptions for medications for concerns like urinary tract infections, and in the event of greater health needs, like high blood pressure, dehydration, malnourishment, or bleeding, the shelter provides free transportation to a nearby hospital where they can receive further care.
“High blood pressure in a dangerous range can lead to preeclampsia,” Haas offered as an example. “If there’s signs of pre-term labor, we send them to a hospital. If they aren’t having normal fetal movement or we cannot find the heartbeat, we send them to get an ultrasound.”

Enedelia Basurto speaks with a group of women at the center.
This type of care allows for mothers to understand their needs in their preferred language to ensure the best care for their pregnancies or post-natal needs. Screening for these common conditions and complications can mean that critical care is provided for individuals and their pregnancies quickly and efficiently, resulting in improved health outcomes for those that come through the Holy Family Birth Center. It can also reduce reliance on emergency rooms, benefiting both the patient and the community. Leone experienced a recent pregnancy that illustrates the importance of their empathetic approach to medicine.
“We had a unique case [the other day] where a group of pregnant women that were all alone came in together. One had a pretty clear cognitive delay… All the women that were with her were looking out for her,” said Leone. “The other women brought her up to me because she [had] started to panic. She traveled alone, she’s a migrant, she has a cognitive delay. It is a hard situation. Ene, Brenda, and I were able to provide good care for her. I was able to calm her down and we were able to get her to the hospital as she had reported some bleeding... The other women were asking about her after making sure she got the care she needed.” Health Network will ensure that her care continues after her hospital visit by arranging prenatal appointments and any other needed follow-up care at a health center near her receiving community, so that after she leaves the border and heads to her new community, she will be immediately linked with care, and her new care team will have records of her treatment at the border. Without this program, the woman would likely not have received any care at the border, with her first opportunity of care when she arrives at her new home, if she can manage to navigate a new health system in a new country on her own.
Read more about this program: Healthy Babies, Children, and Mothers
Read MCN’s white paper on the health needs of pregnant asylum seekers: Failures of US Health Care System for Pregnant Asylum Seekers
Read Annie Leone’s op-ed in STAT News: Devastating Separations Continue for Families Seeking Asylum, with Dire Health Consequences
- Log in to post comments

