Vaccine Acceptance Among Clinicians and What This Means for Refugee, Immigrant, and Migrant Communities
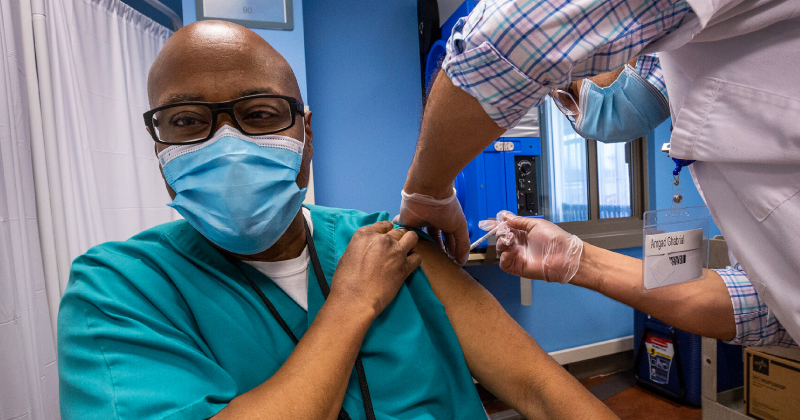
A new paper describing health care worker COVID-19 vaccine confidence and acceptance shows that clinicians who work with immigrant communities were more vaccine acceptant. In Healthcare worker perspectives on COVID-19 vaccines: Implications for increasing vaccine acceptance among healthcare workers and patients, published in Elsevier’s Vaccine journal, authors Christine M. Thomas, Kelly Searle, Erin M. Mann, Jonathan D. Kirsch, William M. Stauffer and MCN's Alma Galván, MCH and Amy Liebman, MPA reported results of a survey conducted with 517 clinicians between March and April 2021. The research and article are the result of a collaborative effort between The National Resource Center for Refugees, Immigrants and Migrants (NRC-RIM) and Migrant Clinicians Network (MCN), funded by the US Centers for Disease Control and Prevention.
The authors surveyed a broad spectrum of clinicians, including anyone involved in the provision of health services, and those who interface directly with patients and those who do not. MCN and NRC-RIM sent the questions to their networks and called on the Society of Refugee Healthcare Providers and a community health center in Florida to further aid with distribution.
The survey found that 88.4% of the clinicians were accepting towards vaccines and, among clinicians who work in refugee, immigrant, and migrant (RIM) communities, that number went up to 95%. Additionally, 138 (36.9%) of clinicians had at least one concern about the vaccines. The most common concern among clinicians was unknown vaccine effects. Almost half of the clinicians also said that recommendations from clinicians were most helpful when talking to hesitant patients about vaccination. Encouragement from trusted sources and educational materials followed in importance according to the clinicians, with around a quarter of the clinicians stating these factors impacted patient acceptance.
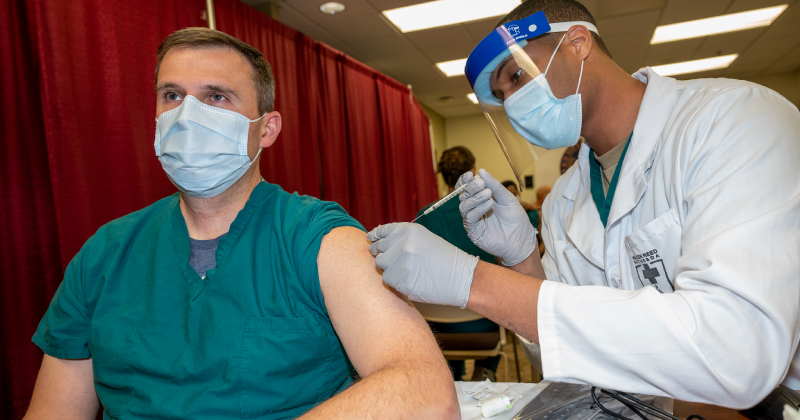
“We took a pragmatic approach to designing the survey and asked questions based on what we would like to know in order to develop practical vaccine-related communications material,” said Christine Thomas, MD, of NRC-RIM. “As a group that seeks to serve RIM communities, we felt there was an invisibility around vaccine perceptions in those communities.” Dr. Thomas believes that by highlighting the importance of the health care provider when it comes to vaccine acceptance, the result of this research “also advocates that we improve access to health care for RIM communities.”
Health care workers have a profound influence in their communities when they discuss health crises like the ongoing COVID-19 pandemic, and this new knowledge reveals the ways that this influence can have positive impacts on patients and communities. The higher acceptance rate of the clinicians who work in RIM communities is promising for provision of care in these populations. Health care workers in RIM communities being among the most positive about vaccination, and the data supporting that clinician acceptance makes patients feel more comfortable accepting a vaccine, mean that they will be able to spread that positivity in key populations. “ The reason for this higher acceptance is unknown but may be that those who provide health care for RIM communities feel a greater sense of social responsibility, tend to work in settings that emphasize disease prevention, or have a deeper appreciation for morbidity and mortality that infectious diseases cause worldwide,” according to the authors.
“It's always helpful to understand what our clinicians are thinking,” said Amy Liebman, MCN’s Director of Environmental and Occupational Health. “These findings have helped, and continue to assist us in shaping the development of our COVID-19 resources and dissemination.”
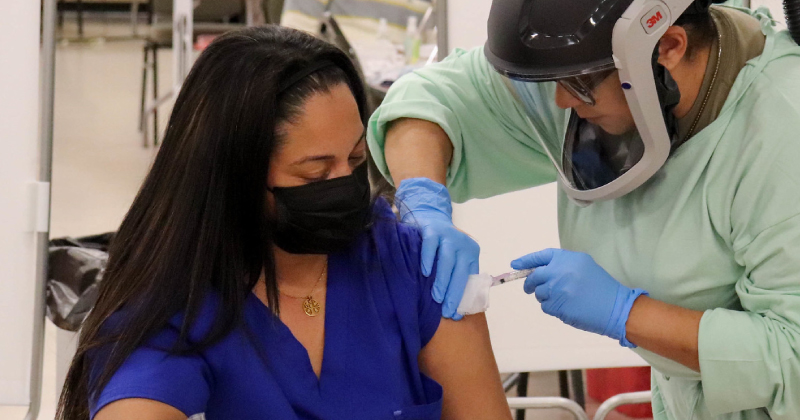
The authors concluded that their “findings also emphasize the importance of prioritizing different methods of messaging for different audiences as health care workers preferred handouts related to frequently asked questions about vaccines for their own decision-making yet indicated their patients may prefer a recommendation from their health care provider.”
Since provider acceptance and recommendation have a positive impact on patient acceptance, a major part of the challenge when it comes to vaccinating RIM communities will come down to getting culturally competent health care workers at the right place at the right time. “In thinking about how these findings can be helpful in the future,” Dr. Thomas explained, “it is in building up health care capacity and access, especially for communities that experience barriers to obtaining health care under the current US model.” The challenges to accessing health care within RIM communities do not exist only around COVID. Many RIM communities struggle to get the care that many others can get more easily. While we address the problems of vaccine hesitancy, we can also address a problem that has existed before the pandemic and that will continue to exist afterward. We need to ensure that all people, regardless of their status as immigrants, refugees, asylum seekers, or migrants, have access to health care. Greater health infrastructure designed to answer the pandemic’s problems can be applied to issues like influenza, diabetes, and a variety of other illnesses that require hands-on care. This pandemic has revealed disparities in our health care system that hurt RIM communities disproportionately, but the work done to survive this pandemic can teach us how to build a better health care system for all of us.
Copies of this paper are available to credentialed journalists upon request; please contact Elsevier's Newsroom at newsroom@elsevier.com or +31 20 485 2719.
You can find resources on vaccination and COVID-19 here:
Our COVID-19 Pandemic Information and Resources page
Our FAQ: COVID-19 and Migrant, Immigrant, and Food & Farm Worker Patients
Got some good news to share? Contact us on our social media pages above.
Return to the main blog page or sign up for blog updates here.
- Log in to post comments
