The Virtual Medical Home at Finger Lakes Community Health
[Editor’s Note: This week, the fall issue of Streamline is arriving in mailboxes across the country. Streamline is Migrant Clinicians Network’s in-print quarterly publication, with clinical updates on emerging issues and best practice from the frontlines. You can subscribe to Streamline for free here. Streamline is seeking new members of its external editorial board. Read about it here. Please contact Claire at cseda@migrantclinician.org if you would like more information. Read the entire fall issue of Streamline here.]
In rural upstate New York, a farmworker heads to the nearby primary care clinic. After check-in, a medical assistant helps him log in with his psychiatrist in the exam room. While the clinic can’t afford to have specialty care in-house, they are able to provide it via telehealth. Instead of driving 45 minutes to get to his appointment, he could reach the provider just a few minutes from his house. And with the cover of the primary care clinic, he can avoid the stigma he was concerned about, around access of mental health care.
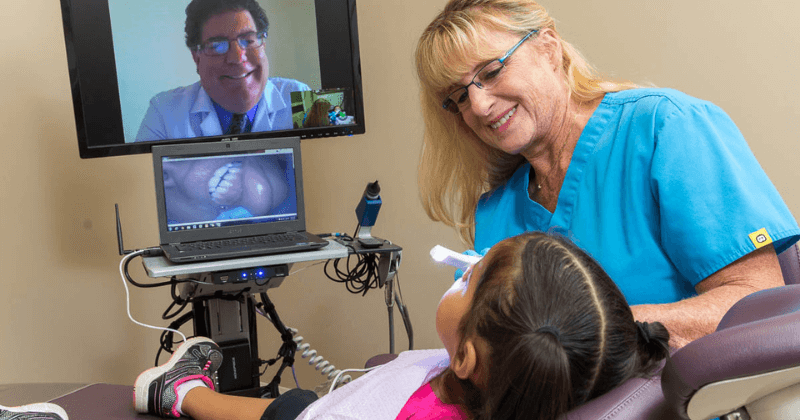
A family couldn’t bring a child in to the pediatric neurologist because of the time off from work and school required to drive for regular appointments, so the neurologist came to them – virtually, in their home. After the medication adjustment made during an after-school appointment, the school reported that the child is doing better academically.
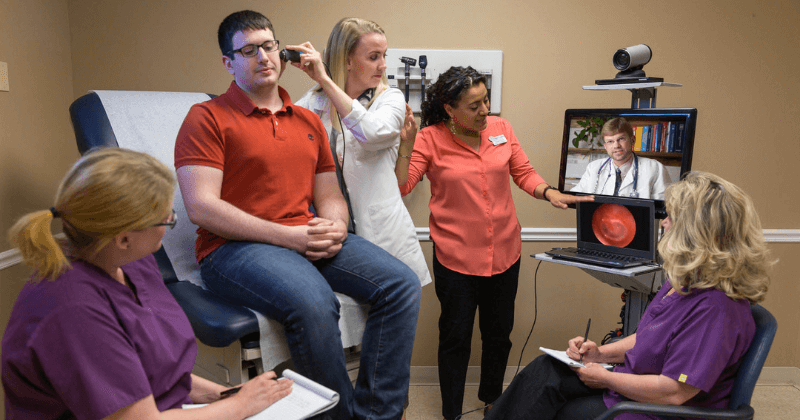
Virtual care via telehealth was given a significant boost during COVID, but some community health centers have embraced telehealth more than others. At Finger Lakes Community Health, the virtual medical home has been a key aspect of their care for over a decade, as the health center’s administration pushed forward telehealth options years before most health centers considered the approach – serving hundreds of patients like the farmworker needing mental health care, and a local child in connecting with a neurologist.
“We saw the virtual health center as an additional site to offer services for our patients,” explained Mary Zelazny, Chief Executive Officer at Finger Lakes, so as early as 2008, she and her team pushed forward specialty care telehealth at their rural clinics, wherein patients could enter the clinic but be seen by a specialty care clinician, who may be hours away in another clinic, through the clinic’s telehealth equipment.
She saw that private practices could bill for telehealth, but community health centers could not – and started to push back. While some limited services were covered, telehealth services were limited by location. After long-time dedicated advocacy, in February 2019, New York State changes its rules, allowing the health center system to bill for telehealth regardless of where the patient was. Finger Lakes clinicians went immediately to work linking rural patients to specialty care that they would otherwise forgo – and the efforts proved particularly beneficial for agricultural workers who had trouble getting to clinical sites.
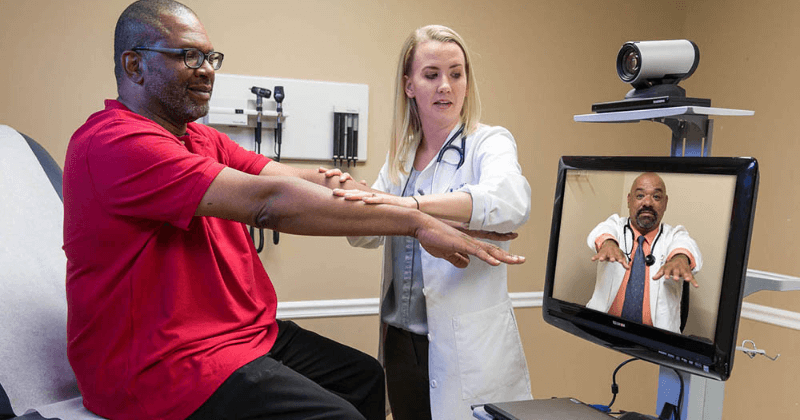
Then COVID hit.
“We were in good shape because we’d been doing it,” Zelazny said. “We already had developed our programs. We were using a HIPAA-compliant platform. We weren’t just willy-nilly turning on the camera – we were very careful from day one.” Even with their telehealth head start, there were hiccups, as providers settled in to providing care at home, and some patients struggled to download the app for their virtual care platform. With subtle differences in the platform depending on how the patient accessed the appointment, whether by cell phone, tablet, or laptop, clinicians struggled on their own to direct patients through. Finger Lakes developed a support team of telehealth specialists – two IT employees, one manager, and one nurse – to support clinicians, and to call patients before their appointment to get their tech in good shape before the provider logged on.
With this COVID-necessitated telehealth revamp, migrant agricultural workers weren’t left behind – in fact, they were ahead of the curve, Zelazny insisted. Providers told her that “the ag workers were a lot more comfortable with video. We think that’s because people were already using Snapchat and WhatsApp to talk to people from home,” Zelazny noted. “They already knew not to move the camera around – they just had a bit more etiquette with the video component. The providers loved having video calls with them because they didn’t get motion sick!”
As COVID funding wanes and clinics return to regular in-person appointments, some health centers have scaled back their virtual operations. That’s a mistake, says Sirene Garcia, Finger Lakes’ Chief Innovation Officer. She sees telehealth as an important way to advance the patient-centered medical home, by bringing primary and specialty care into the same virtual room, for patients who otherwise could struggle to access both. She gives the example of an HIV patient.
“We encourage our providers to sit in on those [specialty care] visits,” she said. The providers share their concerns and talk through the patient’s care plan with each other. “Where else could you have primary and specialty care happening at the same time? And we’re able to pull in [support] for other diseases, like not just HIV but [if the patient] is diabetic as well, [we can] bring all of the folks together and look as a team… to better support” the patient, Garcia said. Of course, reimbursement for such simultaneous encounters can be tricky, but a value-based care model enables clinicians to prioritize the virtual team approach, even when the team is spread out across clinics.

This approach doesn’t just serve the patient – it can lead to growing clinician competence. For example, HIV care was initially not incorporated into primary care. “Fast forward a few years, and it is [now] done in primary care. But when that came about, our providers said, ‘that’s great, I’ll just take a few courses and I’m comfortable’ – because they had been sitting in on those visits… because they were the hands and ears for those specialists,” during telehealth visits.
It’s also an important retention tool. “It’s a career builder, to help our providers have connection with others. Some of our health centers are very small – it can be just one provider. Here, we’re building space for them to talk” with other providers.
Retention is achieved not just at the provider level, but across the clinics. Finger Lakes now employs people in five states – because many don’t need to be in the brick-and-mortar clinic. “We’re increasing our workforce catchment area,” by offering work-from-home opportunities, Garcia noted. “People have moved and we tell them, you can still work for us,” Zelazny says. Finger Lakes is expanding these efforts, with a virtual receptionist program in the works.
With the myriad benefits for patient, provider, and support staff at the clinic, Garcia envisions a growing virtual health center offering, with “one-click access to our health center.” She also envisions not just providers but the entire team working virtually – including financial advocacy and social support for concerns like housing. She’d also like to see more offerings to patients in the home, like increased home visits and shipments of home monitoring equipment like glucometers or blood pressure cuffs. Newer technology can improve home monitoring and make such equipment easier to use for patients.
Garcia believes that with this model, Finger Lakes will best serve patients like agricultural workers who have trouble accessing care otherwise. Her ultimate goal: to “keep pushing the bar, to see how much we can replicate via video that’s done in person,” so that the clinic comes to the patient, rather than the other way around.

Telehealth Policy
Mary Zelazny, Sirene Garcia, and their team at Finger Lakes pushed New York State for better policy to enable telehealth reimbursements at New York community health centers. Each state has unique rules around telehealth including around payment, Medicaid, school-based telehealth, and more. The Center for Connected Health Policy (CCHP) monitors the telehealth policy landscape state by state, and acts as the National Telehealth Policy Resource Center funded by the Health Resources and Services Administration (HRSA). Under that designation, they provide technical assistance to twelve regional Telehealth Resource Centers, state and federal policy makers, and health systems developing or expanding their own telehealth capacities.
Mei Wa Kwong, JD, Executive Director of CCHP, has been watching telehealth initiatives coast to coast as COVID’s temporary telehealth waivers expire. Will health centers still have the same telehealth opportunities? “It’s a mixed bag for clinics,” Kwong said. “They have to consider: are their patients covered by Medicare, Medicaid, out-of-pocket, or a commercial payer?” Each insurance provider will provide different – or no – payments for telehealth. For example, if a state’s Medicaid program does not currently reimburse for telehealth-delivered services, a clinic that has primarily Medicaid patients may have difficulty funding a telehealth program. But clinics with patients with a diversity of payment structures, and clinics especially motivated to provide telehealth due to their patient population, can make it work financially, especially as more policies around telehealth reimbursement are adopted. Each state has its own rules, and many states are presently considering legislation on advancing telehealth. CCHP has tools on its website to find those rules, and track pending regulation and legislation.
Center for Connected Health Policy provides primers on and tracks telehealth policy: https://www.cchpca.org/
National Consortium of Telehealth Resource Centers can direct you to a local resource center: https://telehealthresourcecenter.org/
Data Collection and QI/QA
“We’re going to continue this work – so we need to be able to document everything correctly, and be able to show our payers… and show legislators, that this is the impact that we are [making],” Garcia said. Finger Lakes closely monitors its telehealth outcomes to ensure providers are following compliance requirements, correct codes are used, etc. For their policy push in New York, Finger Lakes tracked their patients with HPV using telehealth versus in-person services, to demonstrate impact and saved costs. “Each telehealth program at Finger Lakes Community Health (FLCH) has a registry of quality metrics based on clinical standards of care,” Zelazny said. “By tracking each element or metric around particular chronic disease or condition, FLCH is able to test the benefits of using technology to address those barriers that a patient might encounter that impedes improved outcomes.”
Visit Finger Lakes Community Health: https://www.localcommunityhealth.com/
- Log in to post comments